Everything you need to know about xenotransplants as US man given pig heart
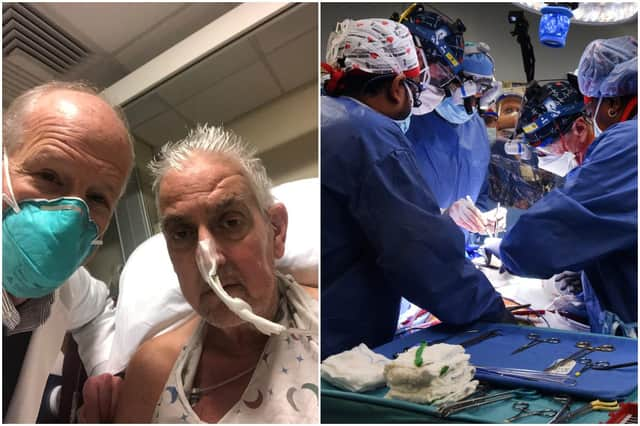

In a medical first, doctors in the USA have transplanted a genetically modified pig heart into a human patient in an effort to save his life.
While too soon to know if the surgery has been a complete success, doctors at the University of Maryland Medical Centre, where the procedure took place, have said that the patient is doing well after the highly experimental surgery.
This is everything you need to know.
What happened in the US?
Advertisement
Hide AdAdvertisement
Hide AdAt the University of Maryland Medical Centre (UMMC), a first of its kind transplant was successfully carried out wherein a 57-year-old man with terminal heart disease received a transplant of a genetically modified pig heart.
The patient, whose name is David Bennett, had been deemed ineligible for a conventional heart transplant, leaving the experimental surgery as his only option. In addition to not qualifying to be put on the transplant list, Mr Bennett was also deemed ineligible for an artificial heart pump due to his arrhythmia.
The day before the surgery, Mr Bennett said: “It was either die or do this transplant. I want to live. I know it’s a shot in the dark, but it’s my last choice.”
On New Year’s Eve, the US Food and Drug Administration (FDA) granted emergency authorisation for the surgery through its “expanded access (compassionate use) provision”.
Advertisement
Hide AdAdvertisement
Hide AdThese are granted when an experimental procedure is the only option left for a patient facing a serious or life threatening medical condition. The UMMC says that this authorisation is given “in the hope of saving the patient’s life”.
Bartley P Griffith, who surgically transplanted the pig heart into Mr Bennett, said: “This was a breakthrough surgery and brings us one step closer to solving the organ shortage crisis.
“There are simply not enough donor human hearts available to meet the long list of potential recipients.
“We are proceeding cautiously, but we are also optimistic that this first-in-the-world surgery will provide an important new option for patients in the future.”
Advertisement
Hide AdAdvertisement
Hide AdAccording to a statement from UMMC, Mr Bennett is “still doing well three days later” after his surgery. He will continue to be carefully monitored over the coming days and weeks.
What is xenotransplantation?
Xenotransplantation refers to a procedure wherein a human is given a transplant/implant/infusion from a nonhuman animal source.
The FDA explains that a xenotransplantation is “any procedure that involves the transplantation, implantation or infusion into a human recipient of either (a) live cells, tissues, or organs from a nonhuman animal source, or (b) human body fluids, cells, tissues or organs that have had ex vivo contact with live nonhuman animal cells, tissues or organs”.
It adds that the development of xenotransplantation has been, in part, driven by the fact that the demand for human organs for clinical transplantation “far exceeds the supply”.
Advertisement
Hide AdAdvertisement
Hide AdThe UMMC said that the donor pig heart underwent a number of gene edits to ensure that it would not be rejected by Mr Bennett.
According to the UMMC, “three genes - responsible for rapid antibody-mediated rejection of pig organs by humans - were “knocked out” in the donor pig”. Six human genes that are responsible for the immune acceptance of the pig heart were then “inserted into the genome”.
“Lastly, one additional gene in the pig was knocked out to prevent excessive growth of the pig heart tissue, which totaled 10 unique gene edits made in the donor pig,” the UMMC said.
What are the risks of xenotransplantation?
The FDA says: “Although the potential benefits are considerable, the use of xenotransplantation raises concerns regarding the potential infection of recipients with both recognized and unrecognized infectious agents and the possible subsequent transmission to their close contacts and into the general human population.
Advertisement
Hide AdAdvertisement
Hide Ad“Of public health concern is the potential for cross-species infection by retroviruses, which may be latent and lead to disease years after infection.
“Moreover, new infectious agents may not be readily identifiable with current techniques.”
Mr Bennett had been fully informed of the procedure's risks, and was informed that the procedure was experimental with unknown potential risks and benefits.
Has xenotransplantation been attempted in the past?
Back in the 1980s, xenotransplants were tried for the first time - however, following a surgery with Stephanie Fae Beauclair, they were largely abandoned.
Advertisement
Hide AdAdvertisement
Hide AdStephanie Fae Beauclair, known as Baby Fae, was born on 14 October 1984 with hypoplastic left heart syndrome.
On 26 October, days after her birth, Baby Fae became the first infant to be subjected to a xenotransplant procedure, as doctors used a baboon heart to replace her own failing heart.
Within a month of the procedure, Baby Fae died - but in her short life, she had, at the time, become the longest living recipient of a non-human heart.
However, since then, pig heart valves have successfully been used for replacing valves in humans for many years.
Is Pig Heart Boy book a true story?
Advertisement
Hide AdAdvertisement
Hide AdPig Heart Boy is a children’s book that was written by Malorie Blackman, and was first published in 1997.
The book tells the story of Cameron, a 13-year-old boy who is in need of a heart transplant when he is offered a highly experimental and controversial surgery in which he would be given a pig’s heart.
Pig Heart Boy is not based on a true story, and is simply a fictional story.